Recently, a major research breakthrough from Shanghai Jiao Tong University School of Medicine on non-invasive neuromodulation for autism spectrum disorder (ASD) was published online inThe BMJ. The study provides an important adjunctive intervention strategy for autism beyond conventional behavioral therapies. The innovative approach was jointly developed over four years through collaboration among Professor Li Fei’s team at Xinhua Hospital, Shanghai Jiao Tong University School of Medicine; Professor Yuan Tifei’s team from the School of Psychology of Shanghai Jiao Tong University and Shanghai Mental Health Center; Professor Cao Aihua’s team from Qilu Hospital of Shandong University; and Professor Fang Shuanfeng’s team from Henan Children’s Hospital. Through a large-scale, high-standard randomized controlled trial (RCT), the researchers demonstrated the intervention’s efficacy, safety, and clinical accessibility. The study was highlighted byThe BMJ as a featured research article and released globally through an international press announcement.
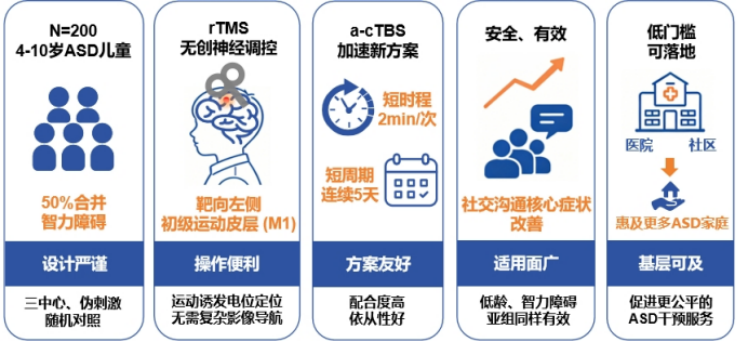
Figure 1. Non-invasive neuromodulation improves social communication deficits in children with autism
Long-Standing Challenges in Autism Treatment
Core social communication deficits in autism have long faced a “no effective medication available” dilemma. To date, no FDA-approved drug specifically targets these symptoms. Traditional rehabilitation and behavioral interventions remain the primary treatment approaches; however, they are often costly and yield highly variable outcomes. Their effectiveness is particularly limited in children with coexisting intellectual disability, despite this group representing one of the most urgent unmet clinical needs.
Repetitive transcranial magnetic stimulation (rTMS), a neuromodulation technique increasingly used in neuropsychiatric disorders worldwide, has shown promising potential for children with autism. Nevertheless, its broader clinical application has been hindered by several barriers, including reliance on expensive and complex neuronavigation systems for target localization, limited accessibility in primary healthcare settings, and difficulties in cooperation among very young children or those with intellectual disabilities. These limitations have contributed to the long-standing lack of diversified treatment options for autism.
Addressing Clinical Pain Points with a Novel Therapeutic Strategy
To overcome the barriers limiting the clinical translation of non-invasive neuromodulation technologies, Professor Li Fei’s team developed and validated an accelerated continuous theta burst stimulation (a-cTBS) intervention protocol.
The protocol targets the primary motor cortex (M1), eliminating dependence on costly neuronavigation systems. Instead, precise localization can be achieved rapidly and objectively through simple electromyographic responses, making the technique feasible for use in grassroots healthcare settings.
In addition, the protocol dramatically shortens treatment duration. Each session lasts only two to three minutes, and the entire intervention course can be completed within five consecutive days. This not only reduces the burden of cooperation for children but also lowers the threshold for clinical implementation, laying the groundwork for broader adoption.
The BMJ simultaneously published a dedicated commentary describing the study as “an important interventional breakthrough in neuroscience,” emphasizing that the protocol’s inclusiveness and practicality make it highly compatible with existing social communication and language-behavioral interventions.
Large-Scale Clinical Validation Fills a Critical Treatment Gap
As the largest randomized controlled neuromodulation trial for autism conducted internationally to date, the study employed a multicenter, randomized, sham-controlled design involving 200 children with autism aged 4–10 years.
Results demonstrated that, both immediately after treatment and at one-month follow-up, children in the intervention group showed significantly greater improvement on the Social Responsiveness Scale (SRS-2) compared with the control group. Core symptoms related to social communication were markedly alleviated, while language abilities also showed positive changes.
Importantly, the protocol demonstrated strong feasibility and therapeutic effectiveness in younger children and in those with coexisting intellectual disabilities, filling a major gap left by previous neuromodulation studies in autism.
Regarding safety, no serious adverse events occurred during the trial. A total of 193 children completed the full treatment course, corresponding to a completion rate of 96.5%, further confirming the intervention’s safety and ease of implementation.
The BMJ also released a visual abstract alongside the publication.
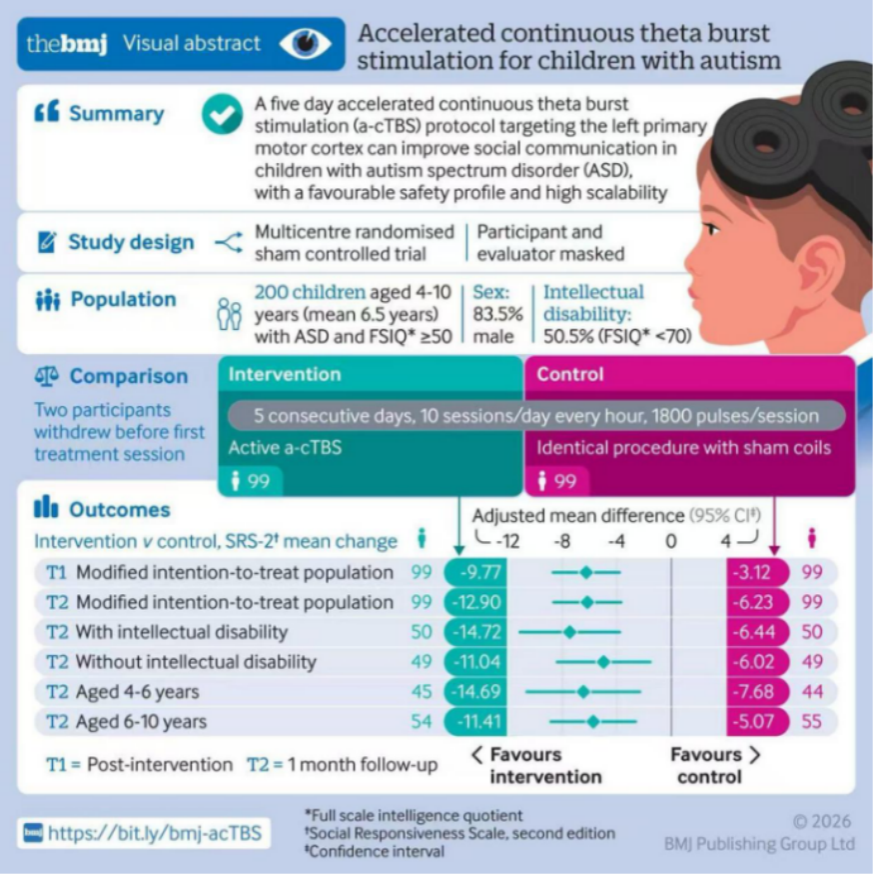
Figure 2. Visual abstract published alongside the study inThe BMJ
Universal Design Makes Advanced Therapy More Accessible to Families
A key strength of the protocol lies in its universally accessible design, ensuring that cutting-edge therapeutic technologies are no longer confined to large tertiary medical centers.
Compared with traditional approaches, the protocol does not require sophisticated localization equipment, significantly reducing implementation costs. The procedure is straightforward and easy to master, with brief treatment sessions and a total course duration of only five days, substantially reducing caregiving burdens and time costs for families.
By lowering implementation barriers, the protocol holds promise for standardized application in remote and economically underdeveloped regions with limited medical resources, thereby greatly improving treatment accessibility.
International experts have highly praised the study, noting that the protocol’s inclusiveness—covering both younger children and those with intellectual disabilities—and its strong clinical feasibility align closely with critical periods of neuroplasticity.
Research into the clinical translation of non-invasive neuromodulation technologies not only provides an additional intervention option for the core symptoms of autism, but also offers technological support for the development of precision intervention systems for neurodevelopmental disorders in China.
From a public health perspective, the protocol may help alleviate shortages of high-quality autism intervention resources and reduce the heavy burden on families by bringing advanced medical technologies into community-level healthcare systems.
The research team also emphasized that current evidence supports the protocol as a potential adjunctive intervention for children with autism, but not as a replacement for established rehabilitation training and educational support. Future research will focus on long-term efficacy and real-world scalability, while promoting integration between neuromodulation technologies and existing behavioral rehabilitation strategies to provide children with autism more diversified, precise, and accessible intervention pathways.
Professor Li Fei’s team at Xinhua Hospital has collaborated extensively with domestic and international experts for more than two decades in the field of pediatric neurodevelopmental disorders, focusing on comprehensive “screening-prevention-diagnosis-treatment-rehabilitation” solutions for children with autism in China.
Previously, the team led the project “Identification and Prevention System for Early-Life Environmental Risk Factors in Neurodevelopmental Disorders,” which received the First Prize of the 2025 Chinese Medical Science and Technology Award.
More recently, the team has achieved a series of landmark breakthroughs in pediatric neurodevelopmental disorders—from major findings on precise gene editing published in Nature to the global release of this non-invasive neuromodulation protocol inThe BMJ—opening new avenues for precision treatment.
Starting from urgent clinical needs, moving toward industrial transformation, and ultimately benefiting the public, this top-tier publication in The BMJ provides a replicable “Shanghai solution” for autism intervention. It also serves as a vivid demonstration of Shanghai Jiao Tong University School of Medicine’s philosophy of “medicine-driven innovation and integration between healthcare and industry.”
At Chuanggu Innovation Park in Yangpu District, the protocol is rapidly transitioning from laboratory research into community-level healthcare applications, building a complete chain of innovation and translational development. Looking ahead, Shanghai Jiao Tong University School of Medicine will continue advancing regional collaborative innovation and help establish a new hub for brain-inspired intelligence and children’s mental health, enabling more original scientific achievements to illuminate the lives of children with autism and bring hope to countless families.

