Shanghai Jiao Tong University School of Medicine (SJTUSM) has actively aligned its efforts with national strategic needs, adhering to the national strategic priorities(known as the “Four Orientations”)and maintaining a problem-driven, mission-orientedresearch approach. The school has systematically advanced mission-oriented scientific research by pooling its resources to conduct original, pioneering investigations. This has continuously enhanced the overall effectiveness of technological innovation. Recently, several research findings from affiliated hospitals have been published in top-tier international academic journals, showcasing the school’s strong innovative momentum in serving public health and advancing medical science and technology.
Research Team Led by Professor Qu Jieming at Ruijin Hospital Publishes inNature Communications:
“Metabolic Regulation” as aPotential Therapeutic Strategy for Bacterial Pneumonia

Recently, the team led by Professor Qu Jieming from the Department of Respiratory and Critical Care Medicine at Ruijin Hospital, an affiliated hospital of Shanghai Jiao Tong University School of Medicine, published a paper titled “Phosphoglycerate Dehydrogenase-Mediated Serine Reprogramming Aggravates Macrophage Hyperinflammation in Murine Pseudomonas aeruginosa Pneumonia” inNature Communications. The paper explores how PHGDH-mediated serine metabolic reprogramming exacerbates excessive macrophage inflammation in the lungs of mice infected with Pseudomonas aeruginosa. Professor Qu Jieming and Associate Researcher Li Yanan are co-corresponding authors of the paper, with Doctoral Students Chen Rong and Zeng Ran serving as co-first authors.
Pseudomonas aeruginosa is a common opportunistic pathogen, particularly prevalent among immunocompromised patients, patients with prolonged hospital stays, or those requiring mechanical ventilation. As one of the major pathogens of hospital-acquired pneumonia, its inherent multidrug resistance and strong biofilm-forming capabilities make clinical treatment extremely challenging, with high mortality rates. The pathological progression of Pseudomonas aeruginosa pneumonia is not only determined by the virulence factors of the bacteria but is also closely linked to the host’s immune response. Macrophages, as the first line of defense in the lungs against pathogen invasion, not only recognize and clear bacteria but also release large amounts of pro-inflammatory cytokines. However, when inflammation becomes excessive or uncontrolled, these cytokines can cause damage to lung tissue, leading to sepsis and even multi-organ failure. Achieving a balance between“effectively clearing pathogens” and“avoiding immune damage” remains a critical challenge in infectious immunology.
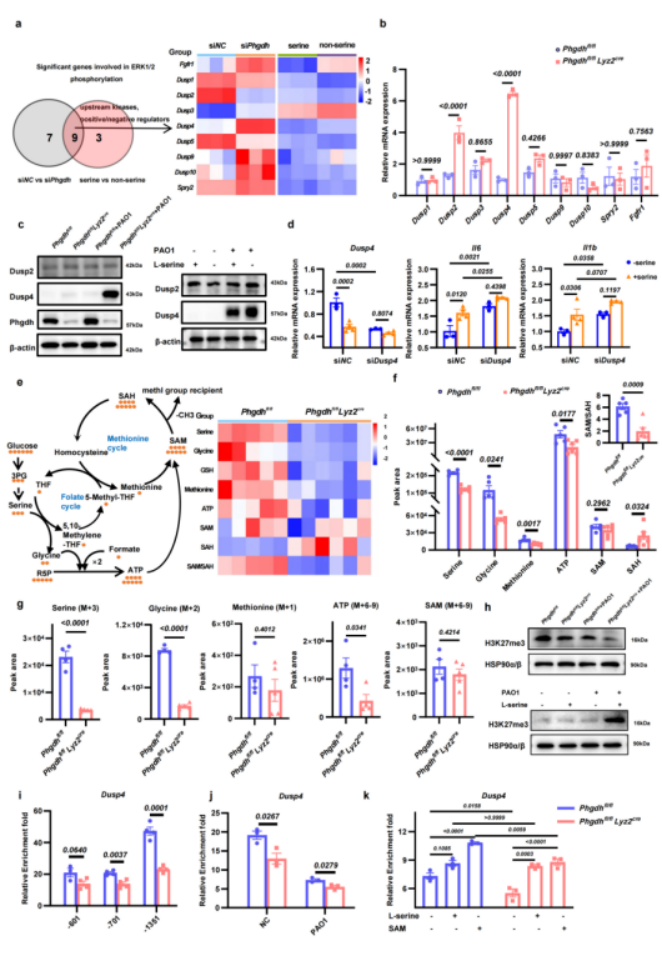
PHGDH-Mediated H3K27me3 Suppresses DUSP4 Transcription
In recent years, accumulating evidence hasshown that macrophage activation state is closely associated with the reprogramming of their intracellular metabolic pathways. As a key component of amino acid metabolism, serine metabolism not only contributes to protein synthesis but also regulates nucleotide biosynthesis, redox homeostasis, and epigenetic modifications through one-carbon metabolism. However, whether serine metabolic reprogramming participates in regulating macrophage inflammatory responses during bacterial infection remains insufficiently understood.
In this study, single-cell RNA sequencing wasused to identify the major cell populations with high phosphoglycerate dehydrogenase (PHGDH) expression, the rate-limiting enzyme in serine biosynthesis, in infected lung tissues. Both in vitro and in vivo macrophage infection models further demonstrated that stimulation by Pseudomonas aeruginosa markedly upregulated PHGDH expression and enzymatic activity. Functional validation using a PHGDH inhibitor and small interfering RNA consistently showed significant suppression of macrophage hyperactivation and pro-inflammatory cytokine release. Moreover, myeloid-specific Phgdh knockout mice were generated to investigate its in vivo role. In a murine model of Pseudomonas aeruginosa pneumonia, knockout mice exhibited significantly improved survival,reduced lung tissue injury, and lower bacterial burden in lung tissues and bronchoalveolar lavage fluid. These changes were accompanied by attenuated depletion of alveolar macrophages and a marked reduction in the proportion of pro-inflammatory macrophages. Mechanistically, integrated analyses including RNA sequencing, metabolic flux assays, and chromatin immunoprecipitation revealed that PHGDH-driven L-serine biosynthesis enhances one-carbon metabolic flux, promotes histone H3 lysine 27 trimethylation (H3K27me3), and facilitates its interaction with dual-specificity phosphatase 4 (DUSP4). This process suppresses DUSP4 transcription and amplifies inflammatory signaling cascades in alveolar macrophages by modulating ERK1/2 phosphorylation.
Research Teams Led by Professors Xue Wei and Pan Jiahua at Renji Hospital Publish inAdvanced Science:
Innovative In Situ cDC1 Vaccine Developed for Prostate Cancer Immunotherapy

Recently, the multidisciplinary team led by Professors Xue Wei and Pan Jiahua from the Department of Urology at Renji Hospital, an affiliated hospital of SJTUSM,published their latest research on prostate cancer immunotherapy in the internationally renowned journalAdvanced Science. The team successfully developed an aptamer-functionalized liposomal delivery platform (Apt-Flt3L@Lipo) that enables targeted co-delivery of FMS-like tyrosine kinase 3 ligand (Flt3L) and chlorin e6 (Ce6). This approach innovatively enables the in situ generation of a cDC1 vaccine, opening a new avenue for the treatment of low-immunogenic prostate cancer.
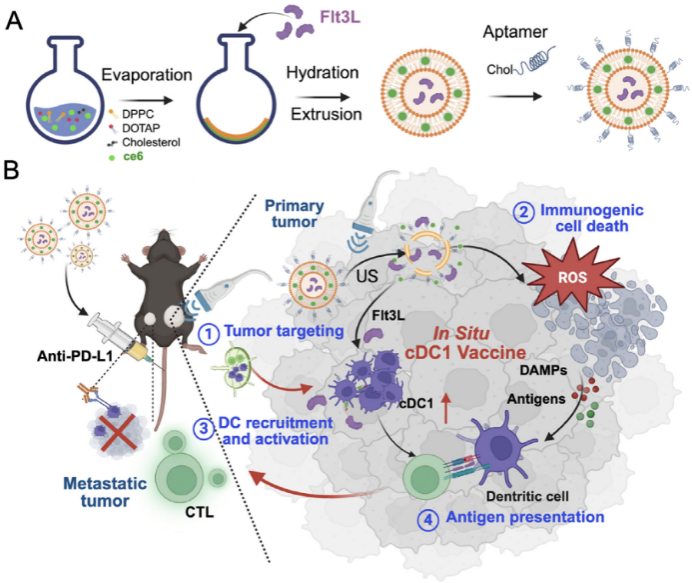
Prostate cancer is the most common malignancy of the male genitourinary system and the second leading cause of cancer-related death among men in developed countries. The 5-year survival rate for patients with advanced disease remains approximately 30%. As a typical“cold tumor,” prostate cancer is characterized by low immunogenicity, a highly immunosuppressive tumor microenvironment, and a marked reduction in both the number and function of conventional type 1 dendritic cells (cDC1), which are essential for antigen presentation. These factors severely limit the efficacy of immunotherapies such as immune checkpoint blockade (ICB), posing a major clinical challenge. Currently approved dendritic cell vaccines require ex vivo manipulation of autologous DCs and are associated with limitations, including a restricted antigen repertoire, complex preparation procedures, and rapid functional decline after reinfusion, thereby limiting their clinical applicability. Therefore, developing novel therapeutic strategiesthat can remodel the tumor immune microenvironment and efficiently activate endogenous antitumor immunity has become a key focus in prostate cancer immunotherapy. The Apt-Flt3L@Lipo platform designed by the research team is prepared through a three-step process involving thin-film hydration, extrusion, and EpCAM aptamer conjugation, enabling precise targeting of prostate tumor tissue via intravenous administration. Upon ultrasound activation, Ce6 induces immunogenic cell death (ICD) in tumor cells,thereby releasing abundant patient-specific tumor antigens. Meanwhile, Flt3L promotes the differentiation and intratumoral recruitment of cDC1 within the tumor microenvironment, achieving precise coupling of antigen release and cDC1 activation. This strategy provides a novel approachto precision immunotherapy in prostate cancer and establishes a theoretical foundation for extending immunotherapy to other low-immunogenic solid tumors, demonstrating strong clinical translation potential.
Dr. Wang Jiayi, a clinical postdoctoral fellow from the Department of Urology at Renji Hospital, is the first author of the study. The co-corresponding authors include Researcher Yang Yu from the Institute of Molecular Medicine, SJTUSM; Professor Xue Wei and Professor Pan Jiahua, Chief Physicians at Renji Hospital; and Associate Researcher Liu Xueliang from the Institute of Molecular Medicine.
Professor Zhao Peiquan’s Team at Xinhua Hospital Publishes Important Findings on Retinoblastoma inJAMA Ophthalmology

Recently, the research team led by Professor Zhao Peiquan from the Department of Ophthalmology at Xinhua Hospital, an affiliated hospital ofSJTUSM, published a significant study titled “Bilateral Conversion Risk in Unilateral Retinoblastoma Using Age and Genetic Testing” online in the prestigious journalJAMA Ophthalmology. The study systematically evaluates the risk of bilateral conversion in children with unilateral retinoblastoma, providing important evidence for clinical precision follow-up and stratified management.
Retinoblastoma is one of the most common intraocular malignant tumors in children. Clinically, some children initially diagnosed with unilateral disease may develop new tumors in the contralateral eye during follow-up. Identifying high-risk individuals early and developing more evidence-based follow-up strategies are key challenges in pediatric ocular oncology.
This study included 1,108 children diagnosed with unilateral retinoblastoma at Xinhua Hospital from July 2010 to October 2024, with a median follow-up period of 43.4 months. The results revealed that 24 children (2.2%) developed metachronous bilateral retinoblastoma duringfollow-up, with most cases occurring within 24 months of the initial diagnosis, suggesting that the first 2 years are a critical monitoring window.
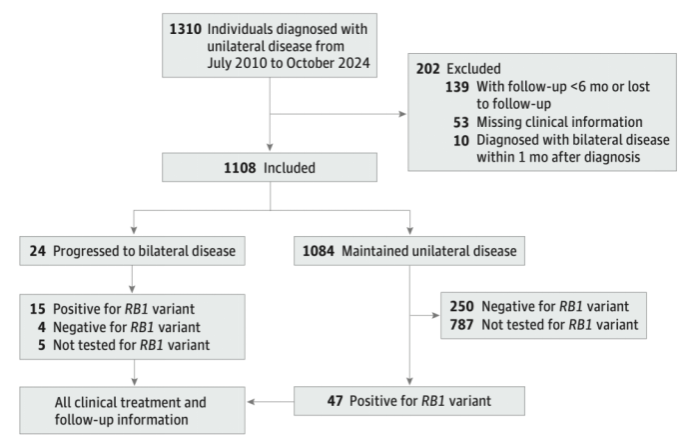
Further analysis showed that peripheral blood RB1 gene testing results were closely associated with the risk of bilateral conversion: the 24-month cumulative incidence in RB1 gene-positive children was 24.8%, significantly higher than the 1.6% in RB1 gene-negative children. Additionally, in RB1 gene-positive children, the age at initial diagnosis was also an important influencing factor. All children who developed bilateral disease were diagnosed before 9 months of age, while no bilateral conversion was observed in children diagnosed at 9 months or older. The study suggests that combining RB1 gene testing with the age at initial diagnosis can more effectively identify high-risk children and provide valuable guidance for follow-up planning, long-term management, and genetic counseling.
In addition to risk prediction, the study also analyzed the intraocular distribution of new lesions in the contralateral eye and found that they were more likely to occur in the nasal and peripheral retinal regions. This finding further supports the key areas for clinical surveillance.

